WHO
四月 23, 2026
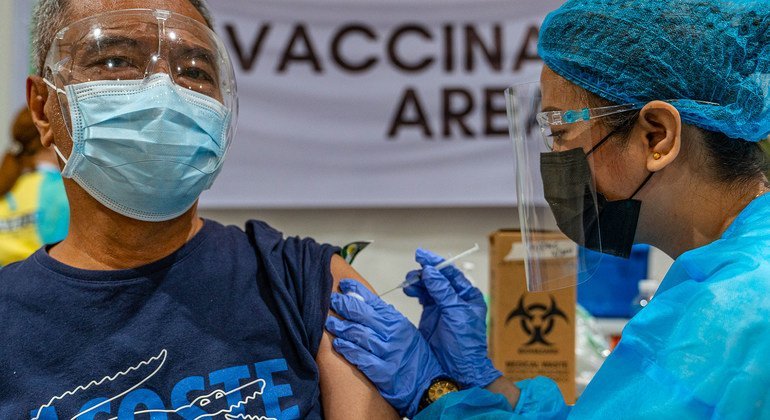
Largest catch-up initiative delivers over 100 million childhood vaccinations
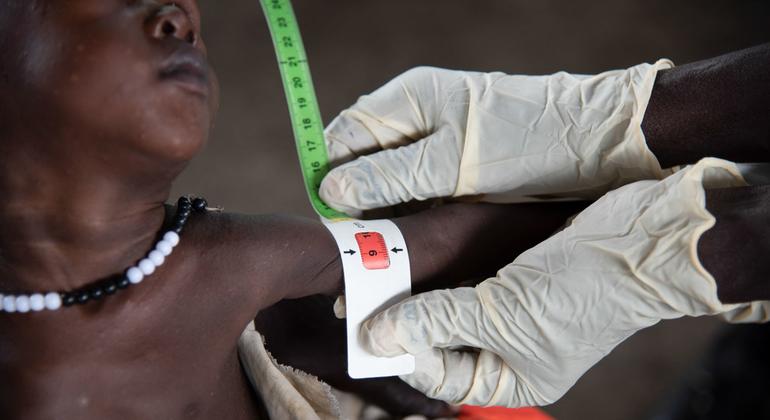
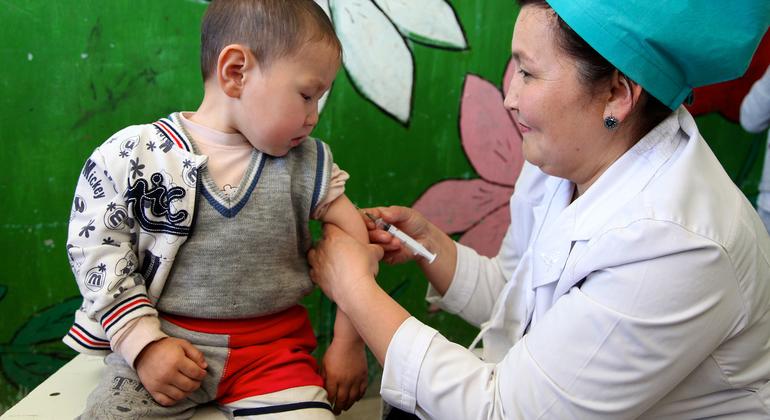
The Big Catch-Up, launched during World Immunization Week 2023, has delivered over 100 million vaccine doses to an estimated 18.3 million children across 36 countriesAround 12.3 million were “zero-dose children” who had not previously received any vaccines and 15 million who had never received a measles vaccine. The initiative concluded in March 2026 and is on track to meet its target of catching up 21 million children – but agencies warn that many infants still miss out on lifesaving vaccines through routine immunization every year.The Big Catch-Up (BCU), a historic multi-year, multi-country effort to address vaccination declines driven largely by the COVID-19 pandemic, has reached an estimated 18.3 million children aged 1 to 5 across 36 countries with more than 100 million doses of life-saving vaccines, helping to narrow critical immunity gaps, announced Gavi, the Vaccine Alliance (Gavi), WHO, and UNICEF at the start of World Immunization Week.Of the 18.3 million children reached between 2023 and 2025, an estimated 12.3 million were “zero-dose children” who had not yet received a vaccine and 15 million had never received a measles vaccine. BCU also provided 23 million doses of inactivated polio vaccine (IPV) to un- and under-vaccinated children, an essential intervention to reach polio eradication. Programme implementation concluded on 31 March 2026. Although final data is still being compiled, the global initiative is forecasted to be on track to meet its target of reaching at least 21 million un- and under-immunized children.However, agencies warn that while catch-up vaccination is an important strategy for closing immunisation gaps, expanding the reach of routine immunization programmes remains the most effective and sustainable way to protect children and prevent outbreaks of vaccine-preventable diseases.Addressing the vaccine equity gapBeyond pandemic recovery, the BCU initiative focused on closing the vaccine equity gap. Millions of children every year miss the essential vaccinations they should receive before the age of one. Most of them live in fragile, conflict-affected, or underserved communities and are never caught up as they grow older.The 36 participating BCU countries across Africa and Asia currently account for 60% of all zero-dose worldwide. Pandemic-related immunisation programme disruptions exacerbated this issue, and, in these countries, added millions more zero-dose children to those who already chronically miss out. To address this issue, the Big Catch-Up looked beyond infant immunization, for the first-time ever systematically leveraging routine immunisation systems to make deep inroads into the accumulated global cohort of older children between the ages of 1 to 5 – “older” because they should have received critical routine vaccines before the age of 1 – who remain vulnerable due to missed vaccinations.BCU catalysed long-lasting systems to identify, screen, vaccinate and monitor coverage rates in these older children – including updates to policies on age eligibility. Countries also oriented and trained health workers to identify, screen and vaccinate missed children as part of routine care and engaged with communities and civil society to support catch-up efforts. By expanding the reach of immunization to millions of previously missed children and their communities, and investing in systemic improvements, the BCU drive has made it easier for the countries to ensure these populations and others like them continue to receive essential health and immunization services in the future.Among the participating countries, 12 countries (Burkina Faso, Democratic People’s Republic of Korea, Ethiopia, Kenya, Madagascar, Mauritania, Niger, Pakistan, Somalia, Togo, United Republic of Tanzania, and Zambia) reported reaching more than 60% of all zero-dose children under the age of 5 who had previously missed DTP1. In Ethiopia, more than 2.5 million previously zero-dose children received DTP1. The country also delivered nearly 5 million doses of IPV and more than 4 million doses of measles vaccine, among other key vaccines, to un- and under-vaccinated children. Countries outside this group also reached large numbers of children. In Nigeria, for example, 2 million previously zero-dose children were reached with DTP1, and 3.4 million doses of IPV were administered alongside millions of doses of other vaccines.While these 36 countries received Gavi funding and technical assistance from WHO and UNICEF through BCU, many other countries also implemented activities during this period to accelerate efforts to catch-up missed children and recover immunisation services following pandemic-related backsliding.“As the largest ever international effort to reach missed children with life-saving vaccines, the Big Catch-Up shows what is possible when governments, partners and communities work together to protect the most vulnerable in society,” said Dr Sania Nishtar, CEO of Gavi, the Vaccine Alliance. “Thanks to this accomplishment, not only are millions of children now protected from preventable diseases but so are their communities, for generations to come.” "By protecting children who missed out on vaccinations because of disruptions to health services caused by COVID-19, the Big Catch-Up has helped to undo one of the pandemic's major negative consequences," said Dr Tedros Adhanom Ghebreyesus, Director-General of the World Health Organization. “The success of the Big Catch-Up is a testament to health workers and national immunization programmes, which are now better equipped to find and vaccinate children missed by routine services." "Vaccinations save lives,” said UNICEF Executive Director Catherine Russell. “This initiative shows what's possible when countries have the resources, tools, and political will to reach children with lifesaving vaccines. We've caught up with some of the children who missed routine vaccinations during the pandemic – but many more remain out of reach. The gains made through the Big Catch-Up must be sustained through investment in strong, reliable immunisation systems, especially at a time where measles is resurging."Looking at the challenges aheadThrough the Big Catch-Up, for the first time ever, countries and global partners successfully reached 12.3 million “older” zero dose children between the ages of 1 to 5. However, in 2024, an estimated 14.3 million infants under the age of one globally failed to receive a single vaccine through routine immunization programmes. Despite BCU demonstrating progress is possible with leadership and targeted investment and support, lowering this annual number of infants who miss out will require building systems that consistently reach the hardest to reach communities – against a backdrop of rising birth cohorts, conflict and displacement, funding cuts, and strained health systems.The consequences of chronic gaps in routine immunisation are plain to see. Measles outbreaks, for example, are rising in every region with around 11 million cases in 2024, and the number of countries facing large outbreaks has almost tripled since 2021. This surge is driven by persistent gaps in measles vaccination through routine immunization programmes, compounded by declining vaccine confidence in some previously high-coverage communities.Large-scale catch-up efforts are resource intensive and should serve only as a gap-filling measure that is complementary to routine immunization. Timely vaccination according to national immunisation schedules provides optimal protection and continues to be the most sustainable way to safeguard children and communities.For every generation, vaccines workWHO, UNICEF, and Gavi, along with countries and communities, are marking World Immunization Week (24–30 April 2026) with a joint campaign, "For every generation, vaccines work," calling on countries to sustain and expand vaccination coverage at every age. At the midpoint of the Immunisation Agenda 2030 (IA2030), and central to Gavi's 2026–2030 strategy (Gavi 6.0), the priority remains the same: reaching zero-dose children and advancing equity in the hardest-to-reach communities, particularly in countries grappling with conflict, instability, or fragile health systems. Maintaining that momentum will require expanding long-term domestic investments in immunization programmes and reliable commitments from partners and donors. Notes to editorsUseful linksPhotos and broll - UNICEFWHO catch up immunisationThe Big Catch-Up: An Essential Immunisation Recovery Plan for 2023 and BeyondAbout Gavi, the Vaccine AllianceGavi, the Vaccine Alliance is a public-private partnership that helps vaccinate more than half the world’s children against some of the world’s deadliest diseases. The Vaccine Alliance brings together developing country and donor governments, the World Health Organization, UNICEF, the World Bank, the vaccine industry, technical agencies, civil society, the Gates Foundation and other private sector partners. View the full list of donor governments and other leading organisations that fund Gavi’s work here.Since its inception in 2000, Gavi has helped to immunise a whole generation – over 1.2 billion children – and prevented more than 20.6 million future deaths, helping to halve child mortality in 78 lower‑income countries. Gavi also plays a key role in improving global health security by supporting health systems as well as funding global stockpiles for Ebola, cholera, meningococcal and yellow fever vaccines. After two decades of progress, Gavi is now focused on protecting the next generation, above all the zero-dose children who have not received even a single vaccine shot. The Vaccine Alliance employs innovative finance and the latest technology – from drones to biometrics – to save lives, prevent outbreaks before they can spread and help countries on the road to self-sufficiency. Learn more at www.gavi.org and connect with us on Bluesky, Facebook, Instagram, LinkedIn, TikTok, X and YouTube.About UNICEFUNICEF, the United Nations agency for children, works to protect the rights of every child, everywhere, especially the most disadvantaged children and in the toughest places to reach. Across more than 190 countries and territories, we do whatever it takes to help children survive, thrive, and fulfil their potential. For more information about UNICEF and its work, please visit: www.unicef.org Follow UNICEF on X (Twitter), Facebook, Instagram, and YouTubeAbout WHODedicated to the health and well-being of all people and guided by science, the World Health Organization leads and champions global efforts to give everyone, everywhere, an equal chance at a safe and healthy life. We are the UN agency for health. We connect nations, partners and people on the front lines in 150+ locations – leading the world’s response to health emergencies, preventing disease, addressing the root causes of health issues and expanding access to medicines and health care. Our mission is to promote health, keep the world safe and serve the vulnerable. www.who.int
Read full article →































































































































































































































































































































































































































































































































































































































/environment-climate-change-and-health-(ech)/_1lc3758.tmb-1200v.jpg?sfvrsn=7d0b6bb8_3)




































































































































































































































































































/sixth-igwg-meeting-on-the-who-pandemic-agreement.tmb-1200v.jpg?sfvrsn=5788659a_1)
































































































































/third-meeting-of-the-intergovernmental-working-group-on-the-who-pandemic-agreement.tmb-1200v.jpg?sfvrsn=b400bf69_6)
/department-of-communications-(dco)/digital-social-visual-(dsv)/who-logo-at-headquarters.tmb-1200v.jpg?sfvrsn=34ba81d2_6)


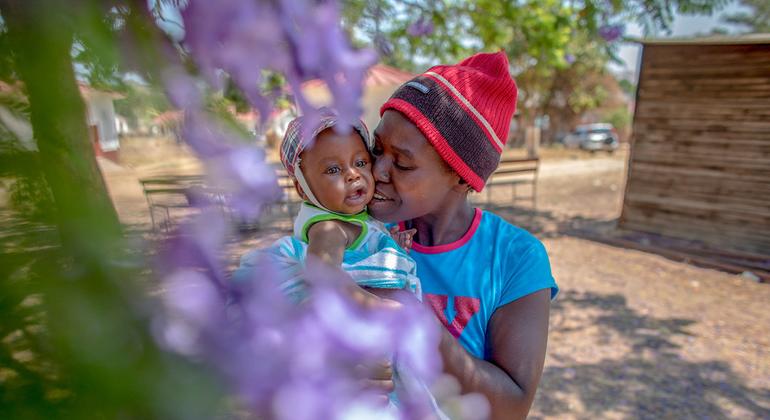




/environment-climate-change-and-health-(ech)/who-photo-scenes-at-fugalei-market.tmb-1200v.jpg?sfvrsn=c265ef9c_7)




/overview-of-igwg4.tmb-1200v.jpg?sfvrsn=3e911e4e_6)